 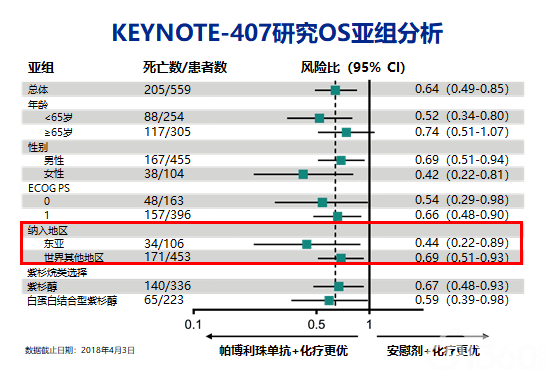
Pembrolizumab was the first PD-1 inhibitor approved by the FDA (Food and Drug Administration) and the first approved for treating previously untreated metastatic NSCLC combined with chemotherapy. 
Patients with PS 3–4 should be offered the best supportive care. For patients with PS of 2, platinum-based doublets should be considered and single agent chemotherapy is an alternative. For patients with PS 0–2 and who are contraindicated for immunotherapy, platinum-based chemotherapy doublets are first-line therapies based on histological subtype and organ function. A combination of platinum-based chemotherapy plus PD-1/PD-L1 inhibitor (e.g., pembrolizumab, atezolizumab) is the most common treatment approach for patients with PS 0–1, regardless of tumour PD-L1 status and without contraindication for ICI. Monotherapy immune check-point inhibitor (ICI) (e.g., pembrolizumab) is the standard treatment for patients with PS 0–1, tumour PD-L1≥50% and without contraindication for ICI. For non-oncogene addicted mNSCLC, therapy is determined by ECOG PS and PD-L1 expression levels. For advanced oncogene-addicted mNSCLC, using agents such as osimertinib, gefitinib, and erlotinib in first-line therapy is recommended. It is recommended that patients are assessed using the Eastern Cooperative Oncology Group (ECOG) Performance Status (PS) before starting any treatment regimen. Especially in the treatment of advanced non-small cell lung cancer (NSCLC), many PD-1/PD-L1 inhibitors have demonstrated satisfactory efficacy and safety.Īccording to the European Society for Medical Oncology (ESMO), in metastatic NSCLC (mNSCLC), the treatment approach varies between oncogene-addicted and non-oncogene-addicted NSCLC. In recent years, programmed cell death protein-1 (PD-1)/programmed death-ligand 1 (PD-L1) inhibitors have drawn much attention in the fields of tumor therapy ( Han et al, 2020). In progression-free survival subgroup analysis, the results demonstrate no significant differences in PFS by PD-L1 TPS expression level, age, liver metastasis status, and smoking status between tislelizumab plus chemotherapy and pembrolizumab plus chemotherapy.Ĭonclusion: The efficacy and safety of tislelizumab combination chemotherapy were not substantially different from pembrolizumab combination chemotherapy. The indirect comparison showed that there was no significant difference between tislelizumab plus chemotherapy and pembrolizumab plus chemotherapy in terms of PFS (HR: 1.04, 95% CI 0.82–1.31), ORR (RR: 0.79, 95% CI 0.59–1.07), the incidence of grade 3 or higher AEs (RR 0.99, 95% CI 0.87–1.12), and AEs leading to death (RR 0.70, 95% CI 0.23–2.09). Regarding safety outcomes, tislelizumab and pembrolizumab have a higher risk in the incidence of grade 3 or higher AEs (RR tis+chemo/chemo 1.12, 95% CI 1.03–1.21 RR pem+chemo/chemo 1.13, 95% CI 1.03–1.24). Direct meta-analysis showed that both treatment regimens improved clinical outcomes compared with chemotherapy alone (PFS: hazard ratio (HR) tis+chemo/chemo 0.55, 95% CI 0.45–0.67 HR pem+chemo/chemo 0.53, 95% CI 0.47–0.60 ORR: relative risk (RR) tis+chemo/chemo 1.50, 95% CI 1.32–1.71 RR pem+chemo/chemo 1.89, 95% CI 1.44–2.48). Results: Data were abstracted from 6 randomized trials involving more than 2,000 participants. Indirect comparisons between tislelizumab and pembrolizumab were conducted with the Bucher method. Methods: We conducted a systematic review of randomized trials the clinical outcomes included overall survival (OS), progression-free survival (PFS), objective response rate (ORR), and adverse events (AEs). Therefore, we conducted an indirect comparison to explore the optimal choice for advanced NSCLC combined with chemotherapy. 
However, no head-to-head clinical trial has ever compared the optimal choice. Purpose: Pembrolizumab and tislelizumab have demonstrated significant clinical benefits in first-line treatment for advanced NSCLC. Department of Pharmacy, Shanxi Province Cancer Hospital/ Shanxi Hospital Affiliated to Cancer Hospital, Chinese Academy of Medical Sciences/Cancer Hospital Affiliated to Shanxi Medical University, Taiyuan, Shanxi Province, China.Yimeng Guo † Junting Jia † Zhiying Hao* Jing Yang* 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
